INTRODUCTION
Surgeons turn to VR as a surgical training tool
It is amazing how technology, specifically virtual reality (VR) is stepping into unimaginable territories such as critical healthcare, playing a pivotal role in training healthcare professionals, enhancing patient care app creation, and improving medical procedures. There was a time when surgeons were evaluated on specialized knowledge alone, while the number of operations they conducted, the success rate, the time taken for a procedure, and their demeanor in the operation room (OR) were all factors that, over time built their repute in professional circles. As technology entered the OR, minimally-invasive surgeries (MIS) such as laparoscopy and endoscopy have turned the focus on skills such as:
- Manual dexterity
- Precise hand-eye coordination
- Quick switches from 3D to 2D visuals (to avoid nausea, eye strain)
- Ability to adapt to the fulcrum effect (inversion of position on monitor)
A skill set that is very different from the demands of traditional open surgery, where senior surgeons supervised and taught trainees, physically guiding their hands when required. With the learning curve steep in MIS, studies of laparoscopic cholecystectomy proved that:
- 90% of common bile duct injuries occurred within the first 30 operations performed by the trainee surgeon.
- The surgeon had a 1.7% probability of causing a bile duct injury in the first operation, which was reduced to 0.17% by the 50th case.
- The probability of injury dropped to a significantly safe level by the tenth case.
- Residency training decreased the likelihood of injuring a bile duct by reducing the frequency of early "learning curve" injuries…a third of which may have been caused by a fundamental error in the technique.
Supervising surgeons realized that VR might help better in bridging the skill gap as the learning curve turned steeper for more complicated procedures like colectomy. A VR environment provides the simulation for a surgical resident not just to learn but also to train in a safe and controlled manner, overcoming the cognitive, visual-spatial, perceptual, and psychomotor challenges posed by MIS technologies.
TRAINING
VR-based surgical training for quality patient care
The rise in the number of aged and sick patients, along with the improvement in critical care services, has led to a situation where experienced surgeons are over-burdened with work, prone to committing errors, and unable to devote time to train apprentice doctors.
The long waiting list for elective surgeries, demand for operation rooms, restricted time slots, and demand for quality care have deprived student surgeons of their rightful hours of experiential learning.
So much so that a recent study found that general surgeons in the US are not universally ready to independently perform core procedures by the time they complete residency training.
Even if a resident surgeon has been to the OR and witnessed a procedure or two, the proficiency level is in question. While expertise can only be gained through exposure and experience, the training is dictated by the location of the hospital, the caseload, case variation, and the teaching prowess of the supervising surgeon.
In answer to all these imponderables, many healthcare innovators have seized the opportunity and have come up with a range of VR surgical training tools, platforms, solutions, and specialized curricula to support surgeons in picking up and honing fresh skills.
Want to know how you can build a VR-based healthcare software?
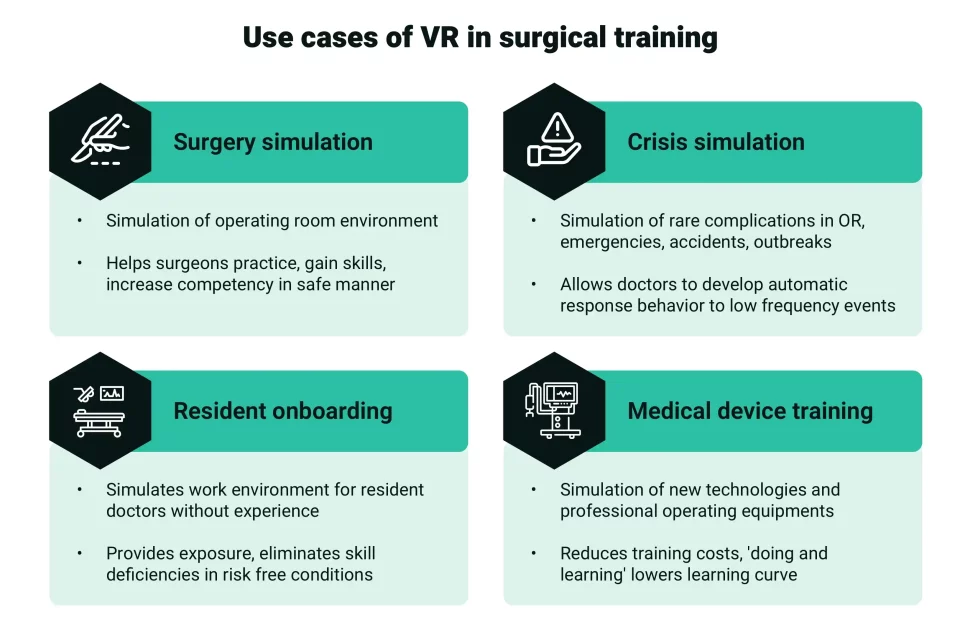 Surgical training with VR-generated simulations is catching on, and hospitals across the world are using it
Surgical training with VR-generated simulations is catching on, and hospitals across the world are using it
INNOVATORS
Startups that provide VR surgical training solutions
VR surgical training tools have long come out of R&D labs and are being used by hospitals worldwide. If some companies offer VR platforms for specific disciplines of surgical training (orthopedics, gastrointestinal, cardiology, pediatrics), others offer VR-based surgical rehearsal platforms for pre-op planning and practice with 3D models, and some others work with experts to develop VR-training curricula for robotic process automation in healthcare sector. Let us take a closer look:
Flight simulator of healthcare
The Queen Elizabeth Hospital in Adelaide, Australia, has deployed VR training in the intensive care unit (ICU) with the aim of standardizing procedures to reduce medical errors and improve patient outcomes.
Instead of spending time and money on organizing workshops, lugging along mannequins, and teaching restrictive “see one, do one, teach one” methodologies, it has sourced VR solutions from a successful clinician-led startup known for its “flight simulator” model for healthcare.
The startup has partnered with many hospitals in Australia; a study has reported a 40% reduction in medical errors, thanks to the VR immersive training tool. The findings of the study are as follows:
- VR-based clinical skills training is viable and provides improved outcomes for learners.
- Improved insights into the nature of human errors in VR training provide benchmarking of human reliability in VR.
- The use of error analyses on a prospective and retrospective basis can help design better VR-based clinician skills training.
Precision VR with haptic feedback
Integration of a kinesthetic and cutaneous haptic system with a VR platform has enabled surgeons to experience accurate physical sensations.
For example, a surgeon who is drilling a bone needs a high level of dexterity, spatial ability, and fine motor skills. If it goes wrong, there is damage to the soft tissue, especially when the drill goes beyond the far cortex -known as a plunge.
It has been demonstrated that the patented haptic system prevents plunge depth by allowing surgeons to feel:
- The vibrations of the drill
- Sensation of the bone texture
- The feeling of the muscle and soft tissue
This force-feedback allows faster build-up of skill mastery and development of muscle memory as the simulations accurately measure angles, depths, and efficiency of movement in a fully immersive training space.
NHS St George’s Hospital in the UK has mandated regular access to this orthopedic simulation training for surgical trainees to accelerate skill transfer.
Next-generation medical training
Going beyond guided and remote coach-led VR surgical training, a leading multi-language VR trainer is venturing into assessments, performance, and outcome-driven training.
Introducing VR-based curricula in orthopedic training procedures, the effort of this company is to establish proficiency thresholds, and prod the time-bound education model of surgical science into a competency-bound reinforcement model.
Inviting early career healthcare professionals to improve surgical prowess “anytime, anywhere” the VR solution aims to democratize access to surgical training and is integrated with:
- Over 25 training modules for ‘on-demand’ learning, which is interactive, with repeatable practice sessions.
- An advanced analytics healthcare tool that benchmarks academic trainee proficiency and tracks performance.
- A curriculum covering an extensive catalog of robotics and complex medical devices to train for “demonstrable” safety threshold in skills.
A similar effort is on in the cardiovascular discipline to democratize access to training in minimally-invasive heart procedures, tie learning to intraoperative metrics and ultimately ensure better patient engagement and health outcomes.
There are many more exciting ventures contributing to the revolution of VR-based surgical training.
TECHNOLOGY
What are the requisites to make a VR environment tick?
An immersive VR surgical training environment comprises a headset, software, hardware, and a computer system.
VR headset: A high-quality headset that acts as an interface between the surgeon and the virtual OR. Provides 360-degree views. Examples -Oculus Rift, HTC Vive, Valve Index, Meta Quest 3.
Head-mounted display accessories: Headphones, microphones, and ergonomic head straps to enhance comfort and distraction-free training.
VR console: A powerful computer that can run VR software and simulations. Robust graphic cards, CPU, RAM, and storage are needed to handle the high computational demand of VR content.
Input devices: Hand-tracking motion controllers, haptic feedback tools, and other user interfaces to help users navigate the virtual environment, interact with objects, and access menus and settings.
Motion tracking systems: External sensors, cameras, and infrared trackers are used to follow the user’s movements within the VR environment and provide accurate positioning data.
Haptic feedback devices: Devices that simulate the sense of touch and force feedback. Examples- gloves, vests, and specialized tools designed to simulate tactile sensations and enhance immersive training experience.
Data tracking, assessment, and analytics tools: Tools designed to collect data on trainee actions, errors, and progress to enable instructors to provide feedback and measure performance.
VR software platform: VR software is created to deploy simulation provide 3D modeling, physics, real-time rendering, and interactivity through a variety of game engines and programming languages. Examples -Unity, Unreal Engine, Python, C/C++, Java, Javascript, HTML5/Web Vr, VR-specific frameworks and SDKs.
Surgical simulations: Specific VR software applications are developed for surgical training and simulation. Examples -anatomical models, medical images, surgical scenarios, and interactive environments to support practice.
Networking and collaboration: If the surgical training solution is collaborative, multiple users are connected with networking tools to allow real-time interactions.
Patient data integration: In some customized VR solutions, patient EHR and other data systems may be integrated to provide patient-specific information for surgical planning and training.
Security, privacy, and technical support: Protecting patient data, ensuring privacy and security of medical records and simulations, content updates and improvements, and troubleshooting problems are a must. Try developing a healthcare cybersecurity plan for robust protection.
Step into the future of healthcare software development with our custom software solutions.
CONCLUSION
VR-trained surgeons will drive healthcare innovation
Though introduced to reduce medical errors and minimize the cost of training, VR-aided surgical training can usher in many futuristic healthcare trends, such as:
- Preoperative planning for personalized surgical procedures,
- Availability of top-tier surgical expertise in remote areas,
- Global collaboration among surgeons and
- Surgeons as co-creators in VR simulations and surgical protocols.
Surely, VR surgical training tools are all set to redefine the healthcare landscape.






